What a year for home health nurse documentation and nurses…
Our COVID song continues…
PDGM has taken over home health nurse documentation…
Home health nurse documentation timeframes are on speed…
And now, Value-Based Purchasing is adding more heat to your already smoke-filled kitchen?!
We started the year with PDGM or the Patient-Driven Group Model as our new payment system.
Then somehow your patient’s “Functional Impairment Score” or “Functional Ability Level” was added to the mix.
And not even 3 weeks ago, it was announced that President Biden approved and made official the ”Home Health Value-Based Purchasing Model” that has been a pilot program in 9 states since 2016.
I’m sure all you’re thinking at this moment is…
- What is all of this?
- Why is it even necessary?
- Which documentation does it have to deal with?
- What does this have to do with me?
- What will I have to change or do?
These are the exact questions I’ll be answering in this post!

Let’s tackle the “what is all of this?”, first…shall we?!
WHAT ARE THE TOP HOME HEALTH NURSE DOCUMENTATION UPDATES OF 2022?
The top home health nurse documentation updates for 2022 are…
- PDGM or the Patient Driven Group Model
- Functional Impairment Scores, or Functional Ability Level, and
- HHVBP or Home Health Value Based Purchasing
Now, no need to read it again, or rush to write it down because you can download the Top Home Health Nurse Documentation Updates for 2022 below.
WHY ARE THESE DOCUMENTATION UPDATES HAPPENING + WHY ARE THEY IMPORTANT?
Medicare was spending astronomical amounts of money on home health services and the patient population wasn’t showing valid improvement in their positive health goals, nor were they reporting receiving quality care, and the rehospitalization rates as well as the fall rates of those same patients that Medicare was footing this astronomical bill for, were increasing even though this astronomical amount of money was being spent on reimbursing providers and home health agencies for the care of these patients.
To place quantities to all of this text, the number of agencies providing home health care in the United States grew from 8,314 in 2005 to 12,613 in 2013 with Medicare expenditures for home health care services alone nearly doubling from 9.7 billion in 2001 to about $18.3 billion in 2012.
And outrageously in 2018, the U.S. home health spending officially hit $102.2 billion.
In comparison, home health care spending growth specifically checked in at 5.2% in 2018. It reached 4.5% and 4.2% in the two prior years, respectively. Meaning Medicare’s home health service bill was steadily increasing without justification or proof of quality services being provided.
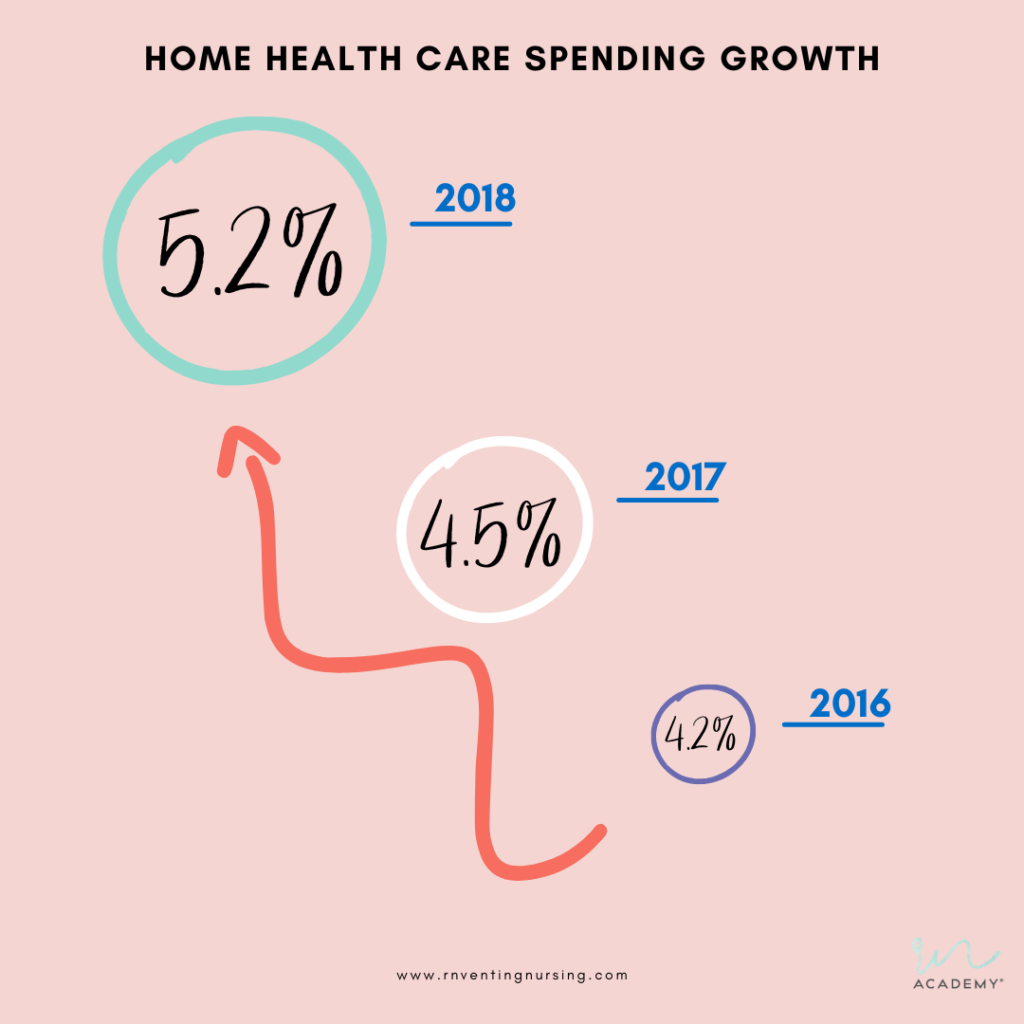
Not to mention, with the way things are going, we are projected to hit $186.8 billion in home health expenditures by 2027.
Needless to say, Medicare needed to figure out a better way to measure, account for, and reimburse for home health services in a way that would increase each patient’s probability of receiving quality care that was actually effective (show me some receipts!!!) and individually focused.
In doing so, the Patient-Driven Group Model or PDGM was created and enacted to…
- Improve the quality of patient care,
- Promote the overall health and well-being of the Medicare Advantage population, and
- Lower healthcare costs.
So instead of your agency getting paid for your nursing visits based on volume metrics, they would be paid based on the value provided to your patients.
The Functional Impairment Score or Functional Ability Level of your patient is actually a piece of the PDGM pie that uses the answers from specific OASIS items in combination with 4 other factors gathered from either your patient’s claim form or their OASIS that calculates their ability to safely function within their home with or without assistance.
You could even think of this score as your patients’ acuity level in order to liken it to a score or level that’s more familiar to nurses outside of home health, and your patients are labeled as having a LOW, MEDIUM, or HIGH functional level.
This score is very important because it sets the stage for the level of assistance, nursing interventions, and frequency of weekly nursing visits you include within their plan of care in order to keep them from injuring themselves or being rehospitalized while under the care of home health services.
In addition to everything that I’ve previously mentioned about your patient’s functional level, it also bears the weight of being the deciding factor of the amount that Medicare ultimately decides to pay your agency for your nursing visits.
HHVBP or Home Health Value-Based Purchasing was initially created as a pilot program to determine if agencies would improve the quality and delivery of their home health services if they were offered reimbursement incentives.
Fortunately, the pilot program that has been going on since 2016 produced some really amazing results for Medicare spending, and the quality of care provided to home health patients, such as…
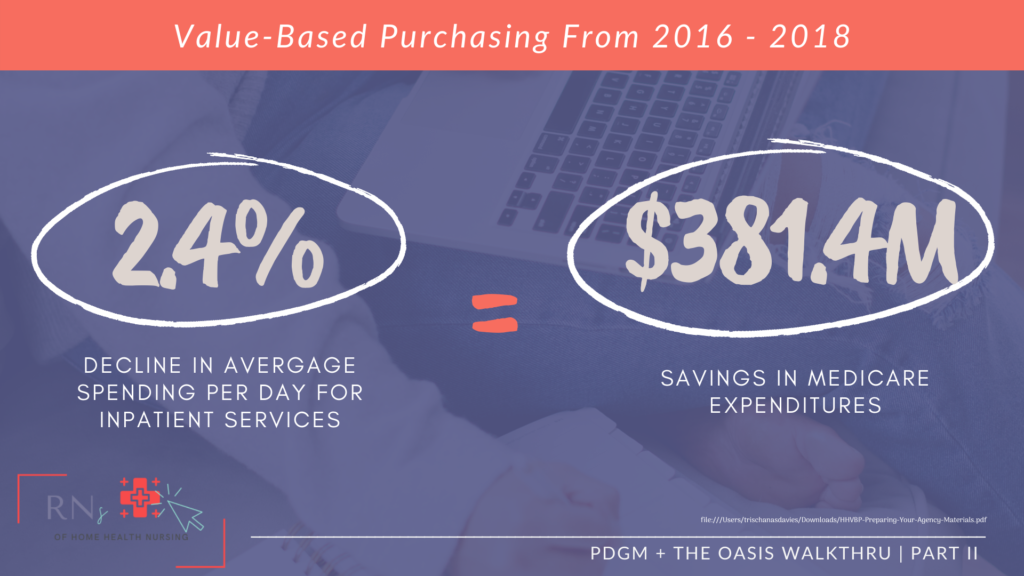
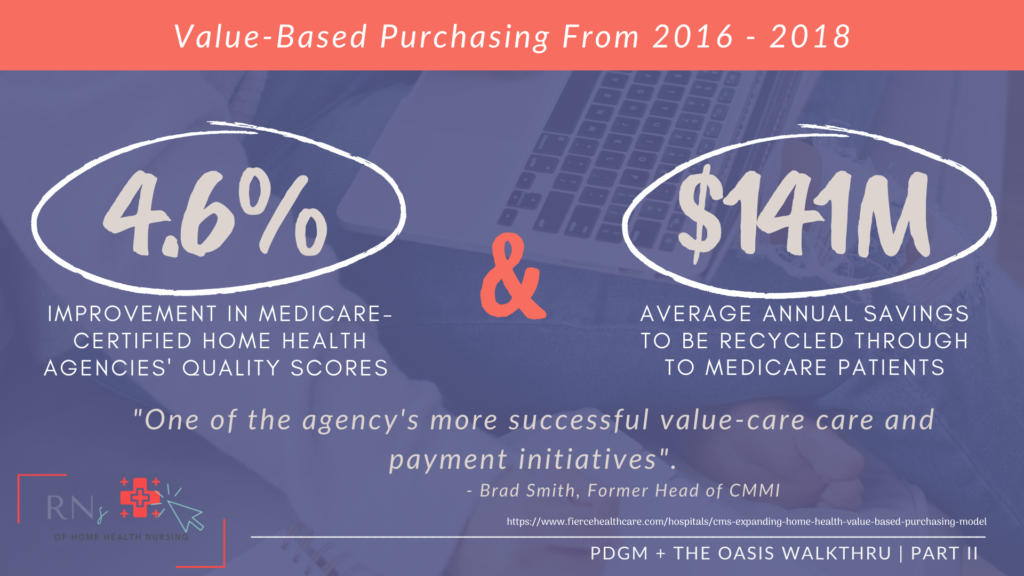

I mean really…need I say more?!
And the story follows with the current HHVBP pilot program ending early to allow a full-fledged HHVBP model to be officially introduced and enacted throughout the entire country, starting in January 2022.
WHICH OF YOUR EVERYDAY NURSING DOCUMENTATION WILL BE AFFECTED?
So this part is going to seem a bit confusing at first, but I promise I’ll break it down and give you a rather SWEET (if I might say so myself…wink) FREE PDF, that you can download below, to pull it all together!
Let’s talk PDGM first.
Everything PDGM is based on Reimbursement Factors, and these factors are basically the specific areas that CMS focuses on when deciding on your agency’s ability to be paid for the nursing visits that you complete with each of your patients.
The current PDGM updates for 2022 are based on 5 Reimbursement Factors, which are your patients’…
- Admission Source
- Episode Timing
- Clinical Grouping
- Functional Level, and their
- Comorbidities( if they have them).
Take a look at the two diagrams below, which have been pulled from our signature course Creating Your Successful EntRNce™ to Home Health Nursing.
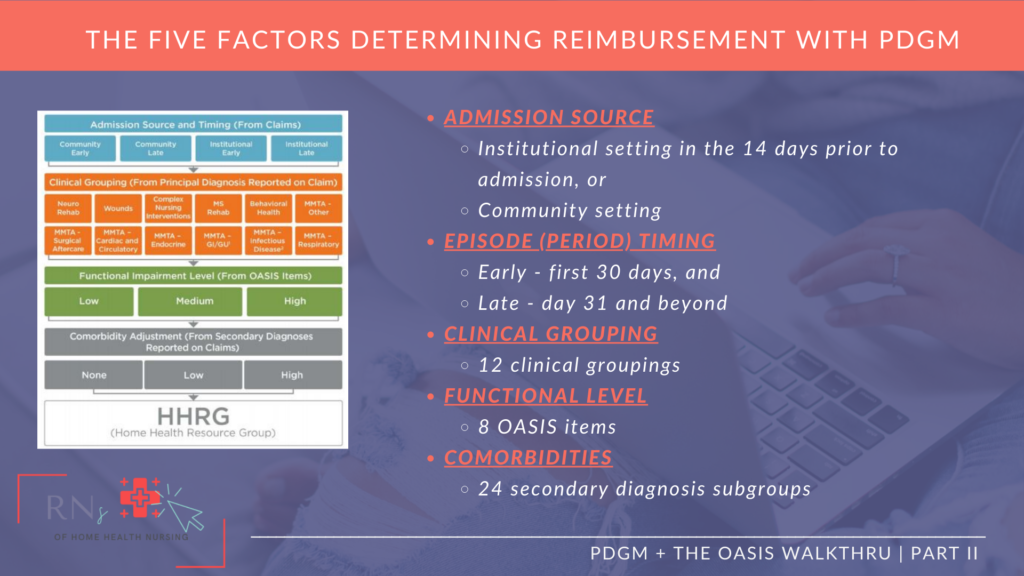
Diagram E shows the definitions for each of the 5 reimbursement factors.
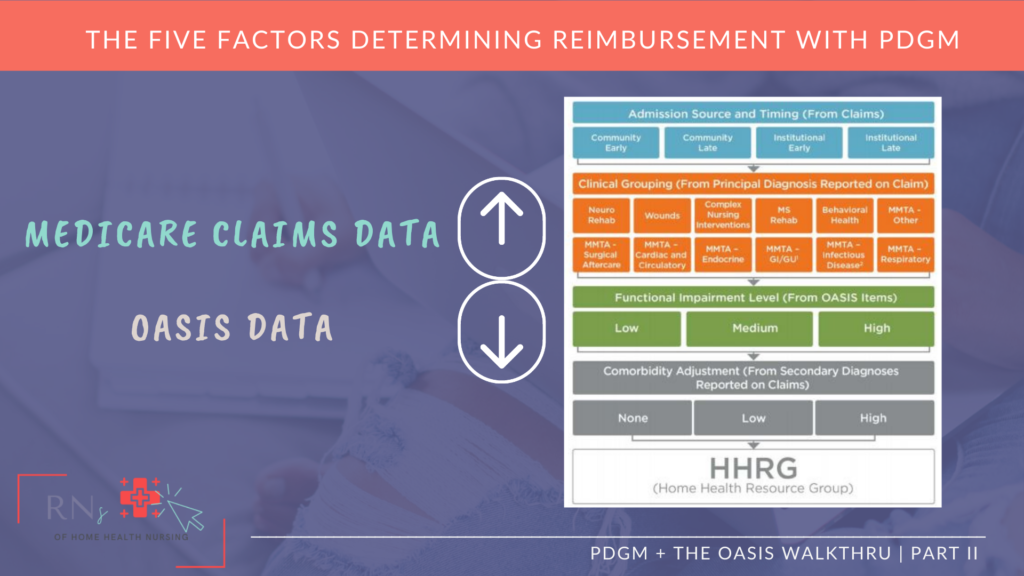
While Diagram F shows you where to find each of the 5 reimbursement factors’ details in order to make nursing decisions and create the proper plan of care.
And
Notice that, “Functional Impairment” (which is what CMS calls it) or “Functional Level/Ability” (which is what nurses call it) is listed in the previous diagrams as one of PDGM’s 5 Reimbursement Factors, which is pretty convenient considering that “Functional Impairment” or “Functional Level” is also the second documentation update for 2022.
No time like the present…let’s jump into the home health documentation changes related to “Functional Impairment”, next.
CMS calculates your patients’ functional level or functional impairment score by their answers to the following 8 specific OASIS items…
- M1033 – Risk of Hospitalization
- M1800 – Grooming
- M1810 – Upper Body Dressing
- M1820 – Lower Body Dressing
- M1830 – Bathing
- M1840 – Toilet Transfer
- M1850 – Bed Transfer
- M1860 – Ambulation/Locomotion
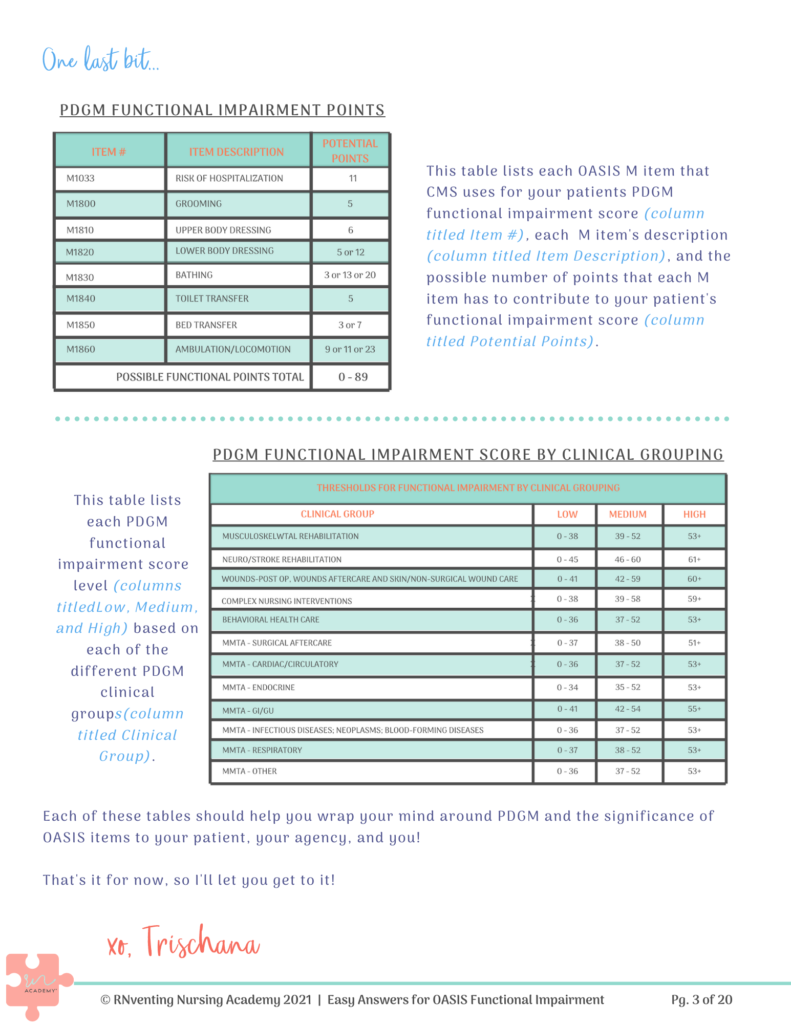
Take a look at the diagram below, that’s been pulled from our PDGM tool Easy Answers™ for OASIS Functional Impairment Guide.
This diagram shows the 8 OASIS items along with their corresponding point possibilities.
With HHVBP or Home Health Value-Based Purchasing, its home health documentation effects are addressed through the same 8 OASIS items as listed above in the Functional Impairment category in addition to the two OASIS items:
- M1845, and
- M1870.
WHO WILL BE RESPONSIBLE FOR COMPLETING THESE NURSING DOCUMENTATION UPDATES?
Given the title of this post, I’m sure you have already gathered that YOU are and will be responsible for the completion and submission of these data updates, but with one really nice caveat being CMS’ new rules of collaboration. Meaning, CMS is now pushing you to not only collaborate with but include the assessment observations of your other agency team members who have assessed the patient within five days of the SOC (if the specific assessment you are completing is a SOC) to determine the most accurate response to each OASIS item.
Now with that being said, you can collaborate with your other agency team members, however, you can only use their assessment data when that particular team member…
- Is “acting or assessing within their scope of practice”,
- Has had “DIRECT CONTACT” with the patient (which can be defined as in-person, health care monitoring devices, video streaming, review of photographs, phone calls, etc.),and
In addition, when you do collaborate with your agency team members and intend to use their assessment data for your OASIS, remember just that…they MUST be from your agency, AND…
- You must document collaboration per your AGENCY POLICY,
- OASIS item M0090-Date Assessment Completed should be updated to reflect the LAST DAY information is collected for OASIS Items or the Comprehensive Assessment, and
- There are restrictions on collaboration for the OASIS PRESSURE ULCER items in M1306-M1324.
In order to keep you on the “straight and narrow” as my father would say, while you’re out in the field or just plain old completing your OASIS assessment documentation, please take the time to download the free ebook below to use as your guidance BEFORE submitting your OASIS documentation to prevent your paychecks from being affected.
You may be thinking, well “why would my paycheck be affected, they can’t do that?!”, just keep reading.
As a quick wrap-up, we’ve covered that the top home health nursing documentation updates for 2022 are…
- PDGM or Patient Driven Group Modeling,
- Functional Impairment Scores, and
- HHVBP or Home Health Value-Based Purchasing
And all 3 of these involve YOU being able to collect the MOST accurate assessment data from your patients for specific OASIS items.
BUUT, what I didn’t already say is that if YOU don’t place the effort into answering those particular OASIS Functional Impairment items ACCURATELY (meaning to the best of your ability given the resources at your disposal and your patients’ situation)…
Your agency could get paid LESS THAN what it ACTUALLY ends up costing to provide care for your patients, which would mean that you just might not end up getting paid PROPERLY for all of the hard work and assessments that you complete on your patients.
Not to mention if your agency gets paid MORE THAN what it costs your agency to provide care for your patients, this is considered FRAUD and YOU and YOUR agency will be investigated and reprimanded accordingly.
So, the best way to ensure that you aren’t fudging your patients’ OASIS answers in either direction unfairly is to…
- Always answer each of your patient’s OASIS Functional Impairment questions as accurately as you can given your situation. Larger entities would say that “making sure that your patient demonstrates and displays every single task to you during their assessment is a MUST”. But I’m here to tell you “You are the feet out there in these streets, you have your patient complete what’s safe and doable”. Besides, there is another really quick way to settle on your patients’ Functional Impairment, and I share that strategy in our course Creating Your Successful EntRNce to Home Health Nursing.
- Follow your gut when assessing your patients and answering OASIS questions, especially as it pertains to the SAFETY of ANY patient.
- Use PHYSICAL THERAPY for collaboration, especially when it comes to answering questions that are in their wheelhouse (like functional impairment). I’m in NO way implying that you don’t have the training or education to assess your patient’s functional ability. But I AM saying that CMS compares what you say versus what physical therapy has to say about each patient during your individual assessments, and if you BOTH aren’t painting the same picture to explain and demonstrate a patient’s “NEED FOR HOME HEALTH CARE SERVICES” then more than likely your agency’s request for reimbursement on that patients’ visits will be denied. This means, your agency will be looking to you to decrease your paycheck for the denied amount or demand you edit your OASIS assessment answers for a resubmission.
- Know the basics of and how to best answer each of the OASIS questions that CMS uses to qualify your agency for the payment of your visits. While understanding that YOU WORK IN REAL-TIME, where patients aren’t always going to bend to your assessment needs or even be able to.
- When and if you collaborate with an agency team member, DOCUMENT, DOCUMENT, DOCUMENT all things pertaining to that collaboration (except opinions…that NEVER goes over well in court!).
I can guarantee there are going to be times when your agency’s quality assurance team or coding department reaches out to you about the way you answered certain OASIS questions, and those times may include them…
- Sending you an email or note through your agency intranet platform, or
- Actually taking it upon themselves to CHANGE your OASIS documentation, or
- Going to your manager to have them pressure you into changing your OASIS answers
In order to have your agency’s reimbursement submission approved. This is and will always be a part of the OASIS documentation submission process, BUUUUUUUUUT I will stand by these next statements with EVERYTHING in my being when I say…
- Anyone other than YOU changing your OASIS documentation IS ILLEGAL because YOU completed the patient’s assessment and those answers are according to YOUR assessments AND YOUR nursing license. So any change that’s not yours can come back to TAKE AWAY OR TARNISH YOUR NURSING LICENSE LATER!
- It is ALWAYS a PRIVILEGE and HEALTHY to get the opportunity to discuss, challenge, and question the views of your QA and coding team members as it pertains to “editing” your OASIS documentation because 1) you will get the chance to view and understand their reasoning behind answering your patients’ OASIS documentation a certain way (and they can add information and details that you may not have been aware of), 2) we are all grown and deserve to be treated as such so asking questions, while giving your point of view is the way to go for a better understanding, and 3) there are NO hard and fast rules that say “once you do gain a better understanding of your QA’s or coding teams suggestion for “editing” your patients’ OASIS documentation, that you can’t then change your answers due to taking the time to better understand your patients’ situation with respect to reimbursement”. The goal here is to GET YOUR PATIENTS’ WHAT THEY NEED TO BE SAFE AND INDEPENDENT IN THEIR HOMES, the goal IS NOT to see who has “the bigger balls”, “more clout”, or whose “right or wrong”. Keep the goal in mind and answering your patients’ OASIS documentation will be smooth.
- And lastly, if you end up “editing” your OASIS documentation, you need to DOCUMENT, DOCUMENT, DOCUMENT why you made changes and per whose suggestion, in a very nice intranet (inner office) email to that person, and keep a copy of that email for yourself.
- ALWAYS remember, that presentation and tact are everything, as my grandmothers’ would always say “You can catch more bees with honey!”, and it’s so true. Present yourself with confidence and approachability, while treating and communicating with others the way you would want to be treated and communicated with…wink!
OKAY, OKAY…I get it, you’re tired of hearing me talk (this has been a rather intense post), but a DEFINITE MUST in order to call myself your “Unapologetic Protector”, and BESTIE in most cases…wink.
As usual, I’ve thrown a TON at you in this post. Along with some true nuggets for you to think about, I’m sure. So do that, think about it, post your questions below, or email me or start a chat in the chat box on my website. Either way, I got you covered 🙂
I’m going to bow out gracefully at this point, but not before I give you one more chance to download the free guide for this post below…
And provide you with actionable steps, of course…
YOUR ACTION ITEMS:
- Take a moment to think through what I’ve shared about the home health nurse documentation updates for 2022, and share your thoughts below in the comments.
- Download the free Top Home Health Nurse Documentation Updates for 2022™ guide to keep the main points of this post at your fingertips when you’re in the thick of it.
- Check out the step-by-step process for answering your OASIS Functional Impairment questions, and creating your patients’ nursing visit frequency schedule accurately in our Easy Answers™ for OASIS Functional Impairment and the included Art of Calculating Nursing Visits™ guides to make this entire process a bit more seamless.
Remember, we RN this together!
Until next time…stay safe 🙂







There’s certainly a lot to learn about this subject.
I really like all the points you made.
Hi Turquise, and welcome to our blog! We are excited to have you :). Yes, there is SO much to learn about home health nursing, but it’s all about baby steps, practice, and understanding yourself enough to know where you need to start in order to learn what’s most important to YOU, along YOUR journey of transitioning to home health nursing, or just plain old nerding out on the topic for fun!!! Either way, I’m here to help you as much as you need ;). Thanks for taking the time to comment, and please stay safe 🙂
I was pretty pleased to discover this page.
I want to to thank you for ones time due to this fantastic read!!
I definitely enjoyed every little bit of it and i also have you saved to fav to look
at new information in your blog.
Hey Pink, it’s so wonderful to have you visiting our blog…WELCOME!! It’s absolutely my pleasure, and this year we have a calendar packed with new fresh reads, free tools, and new products! We’re all about supporting our amazing set of home health nurses who sacrifice so much to care for our communities. This is the least I can do ;). I look forward to hearing from you more throughout the year. Please stay safe 🙂
I in point of fact enjoy the blog article.Really thank you! Awesome.